Uterine Fibroid Embolisation
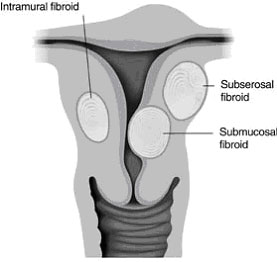
What are Uterine Fibroids?
Uterine fibroids are a troublesome and quite disabling problem for women of childbearing age, until menopause, when they generally regress and become smaller in size. They are the most common tumour of the female genital tract and are thankfully benign.
Some symptoms of uterine fibroids are:
- Chronic pain in the pelvic and/or abdominal regions
- Heavy and/or prolonged bleeding
- Increased urinary frequency and/or urgency
- Constipation
- Abdominal distension or swelling
- Lower back pain
- Pain during intercourse (dyspareunia)
- Infertility or difficulty becoming pregnant
- Problems during pregnancy, including miscarriage
Some 20-40% of women over 35 years of age have uterine fibroids large enough to cause heavy and prolonged menstrual periods. In addition, many of those women also suffer from pelvic pain, constipation, a frequent need to urinate and painful intercourse.
What treatment is available for uterine fibroids?
Treatment for fibroids has traditionally been surgical, necessitating either hysterectomy (complete removal of the uterus) or myomectomy (selective removal of the fibroid tumours by various surgical means). Both techniques require a general anaesthetic and some time spent in hospital.
Recently, uterine fibroids have been treated by a minimally invasive technique known as uterine fibroid embolisation, a procedure performed by an interventional radiologist under local anaesthesia and intravenous sedation. A short inpatient stay of up to 24 hours may be required for post-procedural pain control and observation, however, most patients are able to go home the same day.
How does uterine fibroid embolisation work?
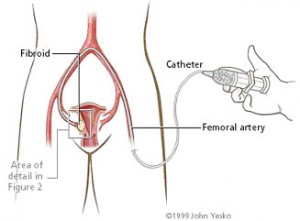
The embolisation procedure is performed by a small puncture made into the artery in the groin known as the common femoral artery.
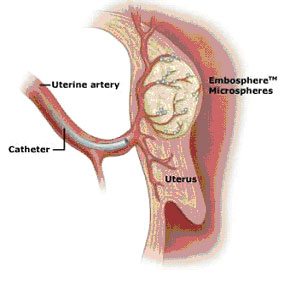
A fine plastic catheter is placed into the artery and directed into the artery supplying the uterus by x-ray guidance. Small particles made of various polymers, gelatin sponge or acrylic beads are directed into the artery supplying blood to the fibroid, blocking it and starving it of oxygen and nutrients.
This ultimately results in destruction of the cells making up the fibroid, with subsequent healing by scar tissue formation and shrinkage of the fibroid.
Is uterine fibroid embolisation a low risk procedure? Can I ask questions beforehand?
The procedure is low risk, with large multi-centre trials now showing significantly better outcomes for women compared to those who had a hysterectomy or myomectomy.
Details of the procedure, peri-procedural investigations and potential problems will be discussed with you at a clinical consultation prior to scheduling your procedure.
You will have an opportunity to ask any questions about the procedure, hospitalisation to follow, as well as any general questions about fibroids you may have.
Will my gynaecologist be kept informed about my procedure?
These findings will then be communicated to your gynaecologist and your procedure will be scheduled at a convenient time for you. Your gynaecologist will be kept informed of your progress at all times.
What happens after the procedure?
About 6 weeks after your procedure, you will be scheduled for a pelvic ultrasound examination to check on the size of the uterus and fibroids.
Is there a fact sheet about the uterine fibroid embolisation and what to expect?
Yes! Find our uterine fibroid embolisation fact sheet here.
What referral form does my doctor need to fill in for a uterine fibroid embolisation procedure?
Fact Sheet
Referral Forms
Contact Us
Procedure Enquiry
Author: Dr John Vrazas MB,BS FRANZCR